Future Applications for Elastography
1 Introduction
New applications of elastography may be grouped into those contingent on technology advances and those related to as-yet-undeveloped clinical applications; the two are interlinked. Because comparisons between pre- and postdistortion images are the essence of strain elastography, any imaging technique can be used for this approach, including magnetic resonance (MR) (see Chapter 12) and optical techniques, notably optical coherence tomography (OCT) and optoacoustic methods. For shear wave elastography, new ways to create the acoustic radiation force impulses and to measure the shear wave speed are being explored.
2 Ultrasound Methods
One application that requires a slow compression is poroelastography, in which the flow of interstitial fluid under compression, which occurs over several seconds, is measured. The clinical analogy is the demonstration of pitting edema, for example, over the ankle, shown by sustained gentle finger compression and then palpation of the resulting pitting of the skin. The problem has been modeled mathematically.1,2 An ultrasound application has been described in transplant kidneys, where steady probe compression and relaxation was applied in 3 second cycles and speckle tracking was used to assess the resulting distortion.3 Significant differences were obtained in the relaxation times compared to the Banff scores indicating differences in edema.
New ways to displace the tissues under examination include sending several acoustic radiation force impulses (ARFIs) from different parts of the array simultaneously. Known as comb push elastography it allows higher frame rates than achievable with a single push pulse. The overlap of several shear waves leads to interference patterns that may reveal new tissue properties.4
The shear waves produced by conventional ARFI push pulses are currently assumed to travel at a single speed, which is used to assess tissue stiffness. But this is a simplification. Actually shear waves occupy a range of frequencies from around 50 to 500 Hz. Those of higher frequencies travel faster than those of lower frequencies (unlike compressional audible sound and ultrasound waves, in which all frequencies travel at the same speed). This phenomenon, known as dispersion, seems to result from properties of the viscous component of the tissue. Understanding how each manufacturer's shear wave system deals with this dispersion could lead to improvements in the spread of reading due to improved consistency across systems.5 Estimation of the dispersion has been shown in ex vivo animal and human studies to allow diagnosis of the amount of fat in the liver and could provide information on the degree of steatosis, which is a major clinical problem.6
The concept of harnessing the shear waves that are generated throughout our bodies by native cardiovascular movements is the subject of active research.7 The challenge is to detect these low amplitude shear waves from noise and to decipher the complex interference patterns produced when they overlap. It could open the way to a wider range of shear wave speed estimations.
3 Optical Methods
Optical coherence tomography (OCT) is powerful technique for imaging superficial structures such as the skin and the eye using laser light at visible wavelengths and a phase-sensitive technique to produce tomograms with submicron resolution. It has become a standard technique for examining the retina and subretinal layers in ophthalmology and can be adapted as a strain elastographic method by comparing OCT scans taken before and after a small distorting force is applied; for example to the cornea by a puff of air (as used to measure intraocular pressure in glaucoma).8 An important potential application is in keratoconus, in which the cornea softens and projects anteriorly. Sufferers experience progressive changes to their refraction, and may be offered laser treatment, which has the disastrous effect of further weakening the cornea.9
Optical coherence elastography has been developed to assess the mechanical properties of the skin in tumors and in burns.10,11 Using a probe with a transparent membrane to contact the skin and apply a distorting force (which could be manual, in a handheld device, or automatic, using a piezoelectric crystal), phantom and clinical studies have been performed. The use of a 1mm thick Elastosil transparent stress sensor plate between the probe and the skin to measure the applied stress allows quantitative estimates of the skin’s elasticity. The trial images have strikingly high strain contrast at submillimeter resolution. If similar stress sensors could be incorporated into ultrasound transducers, quantitative strain ultrasound elastography might become possible.
4 Optoacoustic Methods
When a coherent light beam traverses or is back-scattered from a material that is vibrated mechanically, the movement of the material disturbs the light beam and changes the laser speckle pattern. A camera looking at the laser detects a reduction in the laser speckle contrast. This effect can be harnessed to sense the arrival of a shear wave, forming an alternative detection system to ultrasound with the advantage of better sensitivity than ultrasound offers.
The approach has been developed into an experimental shear wave system in which one or more ARFI pulses are directed into a test object and the time-of-flight of the shear wave is measured optically with great accuracy.12 In the experimental system, the camera watches for the transient reduction in laser speckle contrast while an ARFI pulse is sent into the material some distance to one side; repositioning the ARFI pulse can be used to measure the shear wave speed. Both theoretical models and simulation have been developed for the system. Like all optical systems, it is depth limited and, even using the longer wavelengths of infrared light, only 20 to 30mm of penetration can be achieved, so clinical use would be limited to structures close to the probes such as small parts and endoscopic applications.
5 New Clinical Applications
There are several clinical applications that are being explored but are not yet in clinical use. The literature regarding the most promising of these are summarized below.
5.1 Obstetrics and Gynecology
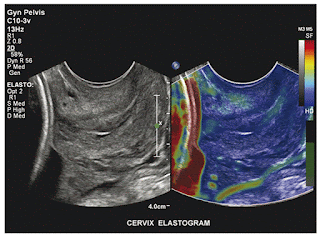
One of the most compelling possible clinical uses is assessment of the softening of the uterine cervix before delivery in late pregnancy (▶ Fig. 13.1). In the normal process, as well as in cervical shortening, there is a reduction in the cervix’s stiffness that allows cervical dilatation to permit passage of the fetal head along the birth canal. These changes are conventionally assessed by a combination of transvaginal ultrasound and manual palpation; these form the basis for the Bishop’s score that is used in obstetric decision-making. If this ripening occurs early, premature delivery is more likely, with devastating consequences for the neonate.
Fig. 13.1 Uterine cervix. Part of the stiff (red coding) fetal head can be discerned on the left of this strain elastogram taken with a transvaginal probe. The endocervix is slightly stiffer than the muscular portion, indicating that ripening has not progressed. (Courtesy of Dr. John MacQuarry, Philips Medical Systems, Bothel, Washington.)
Attempts to use strain elastography have not proved very successful, probably because of the complex structure of the cervix, with intertwined layers of fibrous tissue and smooth muscle, and the difficulty of applying the necessary force uniformly.13 The shear wave approach seems more promising, though this may necessitate the development of special small transducers that can be applied directly to the posterior surface of the cervix via the posterior fornix.14
Another obstetrical application that is promising is in ectopic gestations, where suspicious adnexal masses that proved to be ectopic showed increased stiffness on strain elastography (termed the blue eye sign).15 This was reliable regardless of the β-HCG (beta-human chorionic gonadotropin) level or the conventional ultrasound features.
The stiffness of predominantly cystic ovarian masses has been studied in a small group of patients (26) using transvaginal strain elastography and a subjective scoring system.16 Most lesions showed the mixed pattern suggestive of simple cysts, but 3 of the masses contained stiffer regions and these corresponded to carcinomas, as confirmed on histology. The method could be a useful adjunct to conventional transvaginal assessment when the diagnosis of ovarian cancer is entertained.
Polycystic ovaries (PCO) were found to be stiffer than normal ovaries on strain elastography in a study of 48 patients compared with an equal number of healthy volunteers,16 and the interobserver correlations were excellent. Measurement of ovarian stiffness merits further investigation as a means to improve the diagnosis of PCO in conjunction with ovarian appearance and volume.
A pilot study of over 200 women (some normal and others with a variety of uterine pathologies) using transvaginal strain elastography demonstrated that the normal myometrium had a uniform, stiff appearance that was distinct from the serosa, which presented a laminar pattern.17 Leiomyomas (56 cases, confirmed on histology or MR) were also found to be uniformly stiff but somewhat stiffer than normal myometrium (▶ Fig. 13.2). Adenomyomatosis (11 cases, confirmed on MR) were softer than myometrium with an irregular pattern and margins. Some artifacts that are important to recognize were highlighted in the study, as was the need for practice in order to obtain repeatable results.
Fig. 13.2 Uterus with fibroid. In this transvaginal strain elastogram of the uterus, the myometrium has a uniform, rather stiff appearance while the fundal fibroid (arrowheads) is stiffer and somewhat heterogeneous. (Courtesy of Dr. John MacQuarry, Philips Medical Systems, Bothel, WA.)
In a case report of a women with a leiomyosarcoma compared with another with a simple leiomyoma (fibroid), the malignancy was found to be stiffer on strain and shear wave elastography, both performed using an ARFI method.18 The leiomyosarcoma also showed more heterogeneity of stiffness through the lesion. Larger studies are needed.
5.2 Spleen
The spleen’s mechanical properties are affected by the hemodynamic changes that occur in portal hypertension, and this has been proposed as an alternative to assessing the liver itself, especially where the liver is difficult to evaluate because it is badly damaged and heterogeneous (▶ Fig. 13.3). In a study of 123 patients with varying degrees of liver fibrosis and cirrhosis (mainly attributable to hepatitis C), using the SuperSonic imaging (SSI) shear wave elastography system (Aixplorer, SuperSonic Imagine), spleen stiffness was higher than liver stiffness at all grades.19 A cutoff value between mild and severe liver fibrosis of 23 kPa (cf., 11 kPa for normal liver) is recommended. A high body mass index (BMI) and small spleen size were associated with failed spleen measurements, which were more common than failed liver measurements.
Fig. 13.3 Splenic abscess. A 36-year-old male recently arrived from the Middle East presented with fever and left upper quadrant pain. The B-mode scan (a) showed a well-defined, solid-appearing heterogeneous splenic mass. On ARFI strain elastography, it was found to be of mixed medium-to-soft stiffness (green-to-mauve) in comparison to the surrounding spleen, which was also somewhat heterogeneous. It proved to be a bacterial abscess, caught in the preliquefactive phase. (Courtesy of Prof. Paul Sidhu, King’s College Hospital, London, UK.)
Patients with biliary atresia were studied following a Kasai procedure using an ARFI approach (Virtual Touch quantification [VTq], Siemens) and spleen stiffness was found to correlate with the development of portal hypertension and to predict the need for liver transplantation using a threshold of 2.55 m/s.20 Combining liver and spleen stiffness values improved the predictive value.
Transient strain elastography (TSE, FibroScan, Echosens) and shear wave elastography (SSI, Aixplorer, SuperSonic Imagine) were compared in a well-run prospective study of 79 patients with a variety of diffuse liver diseases of advanced degree.21 A striking finding was the high failure rate of TSE (58% compared with 3% for SSI SWE), mainly attributable to ascites, which is a recognized limitation of the mechanical push used by the FibroScan. However, while the liver measurements were useful at predicting portal hypertension in these cirrhotic patients, spleen stiffness was less useful, though the combination was strongest.
5.3 Neuroectoderm
The brain might seem an unlikely choice of organ for ultrasound elastography, but mapping the increased stiffness of brain tumors to guide brain surgery is of great interest to surgeons, and so intraoperative methods have been developed.22 Meningiomas are stiffer than gliomas.
Another organ whose mechanical properties can be studied with ultrasound (as well as with OCT) is the eye. In a study of 14 eyes blinded by glaucoma, strain elastography was used to assess the stiffness of the optic nerve and of the retrobulbar fat.23 Vibration was applied via the closed eyelids and strain maps developed, from which nerve-to-fat ratios were calculated. Suggested applications include tumors, inflammation, and autoimmune changes, such as occur in Graves’ syndrome exophthalmos. While strain elastography is likely safe in the eye, the push pulses used in ARFI elastography are above the upper limit of the Food and Drug Administration (FDA) recommendations for acoustic power in the eye, so such studies may be unwise, though it has been used experimentally in keratoconus, where it was able to monitor improvements in corneal stiffness after cross-linking therapy.24
5.4 Vascular System
The compliance of arterial and venous walls is an important topic in hypertension and in selecting vessels for grafting and dialysis arteriovenous fistula formation, and it can be measured using ultrasound elastography.25 Thus far it has remained a research tool, but simpler implementations could lead to wider clinical use.
Shear wave elastography has been used for evaluating plaque in the carotid arteries, and here, as in many musculoskeletal applications, it is softer tissue that is pathologic. Soft plaque, thanks to its abundant lipid content, is more vulnerable to rupture and thus is associated with a higher risk of stroke, both using experimental and commercial imaging systems (▶ Fig. 13.4).26,27 That such small structures can be assessed qualitatively for stiffness using ultrasound is a tribute to the sophistication of the technology.
Fig. 13.4 Carotid plaque. This small atheromatous plaque is stiffer than the surrounding artery on shear wave elastography, suggesting it is stable.
The stiffness of a venous thrombus changes as it develops: initially, the thrombus is very soft but if fibrosis occurs as it matures, the thrombus stiffens and measurements of this could be useful to estimate the age of a thrombus28 (▶ Fig. 13.5). Either strain or shear wave approaches could be used.
Fig. 13.5 Thrombus. Following insertion of a PICC, this patient experienced a sense of fullness in the left arm. B-mode ultrasound showed a dilated subclavian vein and there were no signals within it on Doppler. Shear wave elastography showed stiff tissue, indicating that the thrombus had undergone organization. (a) shows the propagation of the shear wave, which can be used as a quality indicator. The stiffness is shown in (b) as averaging 14.7 kPa.
5.5 Miscellaneous
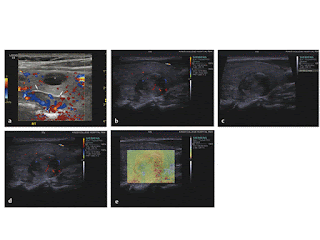
The thyroid has been studied extensively with elastography, in an attempt to reduce the high and unnecessary biopsy rate for thyroid nodules (see Chapter 8), but its use in parathyroid nodules is less well explored.29 However, this could be a useful application because these nodules are typically softer than those of the thyroid. Elastography might confirm the diagnosis in difficult cases, for example, for intrathyroidal parathyroid nodules (▶ Fig. 13.6). It may also be able to alert clinicians to the presence of rare parathyroid carcinoma.
Fig. 13.6 Parathyroid gland. An encapsulated, hypervascular nodule (arrows in a) lying deep to the lower pole of the right lobe of the thyroid is seen in this patient with hypercalcemia; on strain elastography (b), it had intermediate signals, perhaps slightly less stiff than the adjacent thyroid. Its capsule shows as a stiff (blue) region, in keeping with its fibrous nature. There is also an incidental thyroid cyst (asterisk in a), which showed the typical blue-green-red artifact given by fluid. The 15mm nodule indenting the posterior surface of the right lobe of the thyroid gland in (c) had a heterogeneous texture and was moderately vascular on Doppler (d). On strain elastography (e), it had a mixed pattern, with extensive stiff regions (coded in red), which is unexpected for a simple parathyroid adenoma. It proved to a parathyroid carcinoma on biopsy and subsequent excision. ([a, b] Courtesy of Dr. Chris Harvey, Hammersmith Hospital, Imperial College, London. [c, d, e] Courtesy of Prof. Paul Sidhu, King’s College Hospital, London, UK.)
Salivary glands (parotid and submandibular) have been studied in Sjögren’s syndrone;30 normal glands could be completely separated from those with chronic inflammation, and the strain scores correlated well with the B-mode scores, though whether elastography offered any advantage was not made clear.
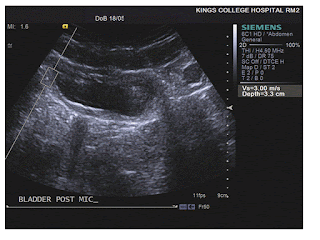
Bladder wall stiffness is a factor in the unstable bladder that is a cause of stress incontinence; attempts to measure it using elastography show promise (▶ Fig. 13.7).31
Fig. 13.7 Bladder wall. In this patient with an overactive bladder, the postmicturition wall shows an ARFI shear wave speed of 3 m/s, consistent with an increase in stiffness that could signify increased muscle tone or to fibrosis.
The development of pressure sores can be predicted by the development of stiffer regions in the deeper layers of ischemic subcutaneous tissue before surface damage is visible.32
Somewhat related is the potential for stiffness estimates in the nasal turbinates, the inferior ones of which are accessible to ultrasound.33 Nasal edema did not affect the results in healthy volunteers. The clinical interest here is in providing a quantitative assessment of the results of surgery.
Monitoring the effects of interstitial therapy is a potential role for shear wave elastography, especially in the liver using thermal techniques such as high-intensity focused ultrasound (HIFU). Coagulated tissue is stiffer than normal, and the higher shear wave speed this produces can be demonstrated with SWE. This could form a practical alternative to contrast-enhanced ultrasound for monitoring interstitial ablations.34
6 Conclusion
New techniques and applications for elastography are promising and could have a major clinical impact.
References
[1] Righetti R, Srinivasan S, Kumar AT, Ophir J, Krouskop TA. Assessing image quality in effective Poisson’s ratio elastography and poroelastography: I. Phys Med Biol 2007; 52(5): 1303‐1320
[2] Righetti R, Ophir J, Kumar AT, Krouskop TA. Assessing image quality in effective Poisson’s ratio elastography and poroelastography: II. Phys Med Biol 2007; 52(5): 1321‐1333
[3] Gao J, Hentel K, Kazam J, Min R. ultrasound strain relaxation time ratio: a quantitative marker for the assessment of cortical inflammation/edema in renal allografts. Ultraschall Med 2015; 41: 112
[4] Song P, Zhao H, Manduca A, Urban MW, Greenleaf JF, Chen S. Comb-push ultrasound shear elastography (CUSE): a novel method for two-dimensional shear elasticity imaging of soft tissues. IEEE Trans Med Imaging 2012; 31(9): 1821‐1832
[5] http://qibawiki.rsna.org/index.php?title=Ultrasound_SWS_Biomarker_Ctte. 2015. Accessed 13 May 2015, 2015.
[6] Barry CT, Mills B, Hah Z et al. Shear wave dispersion measures liver steatosis. Ultrasound Med Biol 2012; 38(2): 175‐182
[7] Brum J, Catheline S, Benech N, Negreira C. Quantitative shear elasticity imaging from a complex elastic wavefield in soft solids with application to passive elastography. IEEE Trans Ultrason Ferroelectr Freq Control 2015; 62(4): 673‐685
[8] Schmitt J. OCT elastography: imaging microscopic deformation and strain of tissue. Opt Express 1998; 3(6): 199‐211
[9] Ford MR, Dupps WJ Jr, Rollins AM, Roy AS, Hu Z. Method for optical coherence elastography of the cornea. J Biomed Opt 2011; 16(1): 016005
[10] Wang RK, Sampson DD, Boppart SA, Kennedy BF. Special section guest editorial: optical elastography and measurement of tissue biomechanics. J Biomed Opt 2013; 18(12): 121501
[11] Es’haghian S, Kennedy KM, Gong P, Sampson DD, McLaughlin RA, Kennedy BF. Optical palpation in vivo: imaging human skin lesions using mechanical contrast. J Biomed Opt 2015; 20(1): 16013
[12] Cheng Y, Li S, Eckersley RJ, Elson DS, Tang MX. Detecting tissue optical and mechanical properties with an ultrasound modulated optical imaging system in reflection detection geometry. Biomed Opt Express 2015; 6(1): 63‐71
[13] Myers KM, Feltovich H, Mazza E et al. The mechanical role of the cervix in pregnancy. J Biomech 2015; 48(9): 1511‐1523
[14] Feltovich H, Hall TJ, Berghella V. Beyond cervical length: emerging technologies for assessing the pregnant cervix. Am J Obstet Gynecol 2012; 207(5): 345‐354
[15] Gazhonova VCS, Zubarev A. Real-time sonoelastography improved early detection of ectopic pregnancy. Paper presented at the European Congress of Radiology (ECR); March 4–8, 2010; Vienna, Austria
[16] Ciledag N, Arda K, Aktas E, Aribas BK. A pilot study on real-time transvaginal ultrasonographic elastography of cystic ovarian lesions. Indian J Med Res 2013; 137(6): 1089‐1092
[17] Stoelinga B, Hehenkamp WJ, Brölmann HA, Huirne JA. Real-time elastography for assessment of uterine disorders. Ultrasound Obstet Gynecol 2014; 43(2): 218‐226
[18] Furukawa S, Soeda S, Watanabe T, Nishiyama H, Fujimori K. The measurement of stiffness of uterine smooth muscle tumor by elastography. Springerplus 2014; 3: 294
[19] Grgurevic I, Puljiz Z, Brnic D et al. Liver and spleen stiffness and their ratio assessed by real-time two dimensional–shear wave elastography in patients with liver fibrosis and cirrhosis due to chronic viral hepatitis. Eur Radiol 2015; 25(11): 3214‐3221
[20] Uchida H, Sakamoto S, Kobayashi M et al. The degree of spleen stiffness measured on acoustic radiation force impulse elastography predicts the severity of portal hypertension in patients with biliary atresia after portoenterostomy. J Pediatr Surg 2015; 50(4): 559‐564
[21] Elkrief L, Rautou PE, Ronot M et al. Prospective comparison of spleen and liver stiffness by using shear-wave and transient elastography for detection of portal hypertension in cirrhosis. Radiology 2015; 275(2): 589‐598
[22] Chauvet D, Imbault M, Capelle L et al. in vivo measurement of brain tumor elasticity using intraoperative shear wave elastography. Ultraschall Med 2015 April 15 [Epub ahead of print]
[23] Vural M, Acar D, Toprak U et al. The evaluation of the retrobulbar orbital fat tissue and optic nerve with strain ratio elastography. Med Ultrasound 2015; 17(1): 45‐48
[24] Urs R, Lloyd HO, Silverman RH. Acoustic radiation force for noninvasive evaluation of corneal biomechanical changes induced by cross-linking therapy. J Ultrasound Med 2014; 33(8): 1417‐1426
[25] Biswas R, Patel P, Park DW et al. Venous elastography: validation of a novel high-resolution ultrasound method for measuring vein compliance using finite element analysis. Semin Dial 2010; 23(1): 105‐109
[26] Ribbers H, Lopata RG, Holewijn S, Pasterkamp G, Blankensteijn JD, de Korte CL. Noninvasive two-dimensional strain imaging of arteries: validation in phantoms and preliminary experience in carotid arteries in vivo. Ultrasound Med Biol 2007; 33(4): 530‐540
[27] Ramnarine KV, Garrard JW, Kanber B, Nduwayo S, Hartshorne TC, Robinson TG. Shear wave elastography imaging of carotid plaques: feasible, reproducible and of clinical potential. Cardiovasc Ultrasound 2014; 12: 49
[28] Wang C, Wang L, Zhang Y, Chen M. A novel approach for assessing the progression of deep venous thrombosis by area of venous thrombus in ultrasonic elastography. Clin Appl Thromb Hemost 2014; 20(3): 311‐317
[29] Ünlütürk U, Erdoğan MF, Demir O, Culha C, Güllü S, Başkal N. The role of ultrasound elastography in preoperative localization of parathyroid lesions: a new assisting method to preoperative parathyroid ultrasonography. Clin Endocrinol (Oxf) 2012; 76(4): 492‐498
[30] Iagnocco A, Iorgoveanu V, Priori R. Involvement of salivary glands in primary Sjögren's syndrome: elastographic assessment and correlations with ultrasonographic findings. Ann Rheum Dis 2014; 73(2): 474‐475
[31] Ying H, Da L, Luo J et al. Quantitative assessment of bladder neck compliance by using transvaginal real-time elastography of women. Ultrasound Med Biol 2013; 39(10): 1727‐1734
[32] Deprez JF, Brusseau E, Fromageau J, Cloutier G, Basset O. On the potential of ultrasound elastography for pressure ulcer early detection. Med Phys 2011; 38(4): 1943‐1950
[33] Kısmalı E, Göde S, Turhal G, Öztürk K, Rașit M. A new insight for evaluation of the inferior turbinate with ultrasound elastography. J Ultrasound Med 2015; 34(5): 777‐782
[34] Hoyt KPK, Rubens DJ. Sonoelastographic shear velocity imaging: experiments on tissue phantom and prostate. IEEE Ultrason Symp. 2006:1686–1689.





Không có nhận xét nào :
Đăng nhận xét