| Purpose: Increased intracranial pressure (ICP) is one of the prevalent symptoms of trauma, especially traumatic headache, which requires quick action for the diagnosis and treatment. The optic nerve sheath diameter (ONSD) is a newly proposed technique for the detection of an increase in ICP. The aim of this study was to assess the efficacy of this new diagnostic method in patients with increased ICP induced by trauma. Methods: This prospective study was conducted between December 2016 and February 2017. The patients with traumatic headache and who had been diagnosed with increased ICP using clinical signs and computed tomography scan were compared to the voluntary healthy group. In each patient, measurements were performed employing ultrasound three times on each eye in an axial region, and the mean of these sizes was obtained as the ONSD. Results: A total of 112 participants were examined. The mean ONSD measurement of the patients and the voluntary healthy group was 6.01 ± 0.76 and 3.41 ± 0.56 mm in the right eye, 6.11 ± 0.75 and 3.39 ± 0.54 mm in the left eye, and 6.06 ± 0.75 and 4.02 ± 1.07 mm in both sides, respectively. The ONSD in the right and left sides had high and significant correlation in the patients (r = 0.929, P < 0.000) and voluntary healthy (r = 0.630, P < 0.000) group. The mean ONSD of one of the patients was 6.24 ± 0.56 mm, and in another patient with no clinical sign of increased ICP, the mean ONSD was 4.61 ± 0.09 mm. Conclusions: Ultrasound performed on the diaphragm of the optic nerve with acceptable sensitivity can detect patients with an increase in ICP and can be efficacious in expediting the action needed to reduce ICP. Due to the sensitivity and specificity of the ultrasound and high accuracy of the diameter of optic nerve sheath in detecting increase in ICP, as well as considering the fact that ultrasound is a noninvasive and available technique; it can be performed at the patient's bedside. | |
Tổng số lượt xem trang
Thứ Năm, 27 tháng 6, 2019
ONSD detects Increased Intracranial Pressure
Thứ Bảy, 22 tháng 6, 2019
5 trends shaping the future of global ultrasound
By Simon Harris, AuntMinnie.com contributing writer
June 17, 2019 -- 2018 was a record year for the world ultrasound equipment market, with revenues increasing by 6.8%, tipping the market over the $7 billion mark for the first time. Despite the backdrop of global economic uncertainty, the ultrasound market is forecast to continue to grow relatively strongly in the coming years, with the following five trends driving growth.
1. Ultrasound attracts new users
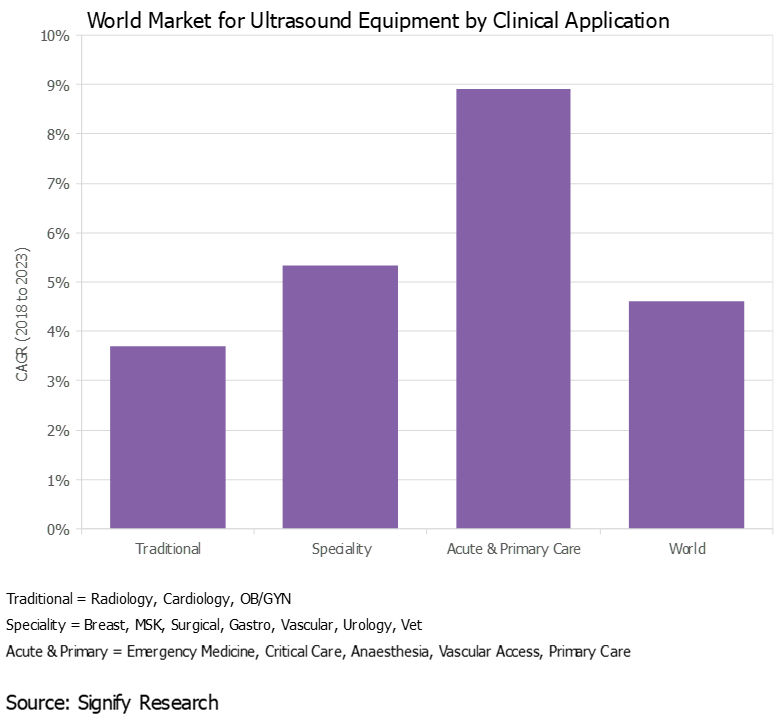
Over the years, the use of ultrasound has gradually expanded beyond radiology, cardiology, and ob/gyn to a wide range of clinical specialties, including surgery, musculoskeletal, and gastroenterology, to name a few, expanding the customer base and driving additional revenue growth.
This trend started out in developed countries, but more recently it has spread to developing markets, particularly India and China, where specialty departments at larger hospitals now often have their own budgets to buy ultrasound scanners.
Additionally, ultrasound is gaining acceptance in acute and primary care settings as both a screening and diagnostic tool, as well as for procedure guidance. With the use of handheld ultrasound gaining pace (see trend No. 4 below), this trend will accelerate in the coming years.

All images courtesy of Signify Research.
2. New clinical applications evolve
Along with the growing customer base, the use of ultrasound with existing customers is expanding, typically as a lower-cost and/or radiation-free alternative to other imaging modalities, such as MRI and CT. The global shift to value-based care as a replacement to the traditional fee-for-service approach will support this trend.
For example, ultrasound is playing an increasingly important role as a screening tool for women with dense breast tissue. In acute care, ultrasound is increasingly being used for lung imaging to diagnose conditions such as pleural effusion, pulmonary edema, and pneumothorax. In another example, the use of shear-wave elastography is expanding beyond hepatology (e.g., liver fibrosis) to other body areas, including the breast, prostate, thyroid, and spleen. Musculoskeletal imaging is another relatively untapped market for ultrasound, including orthopedics, rheumatology, and sports medicine.
3. New markets emerge
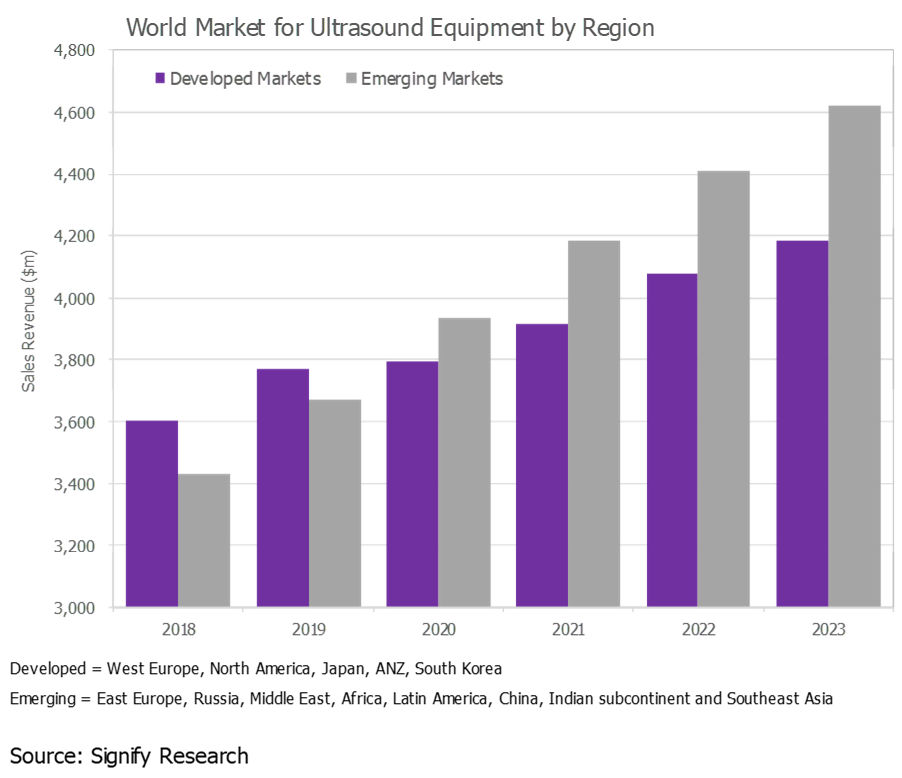
The ultrasound market in developed regions, such as Western Europe, North America, and Japan, is largely saturated, and the outlook is for low-single-digit to midsingle-digit growth. While these markets will continue to account for the lion's share of the world market, developing markets continue to represent a growth opportunity. In 2019, the fastest growth is forecast for Southeast Asia, Brazil, China, and India.
That said, ultrasound market growth is slowing in many of the emerging markets, particularly China, largely due to slowing global economic growth.

4. Handheld ultrasound picks up steam
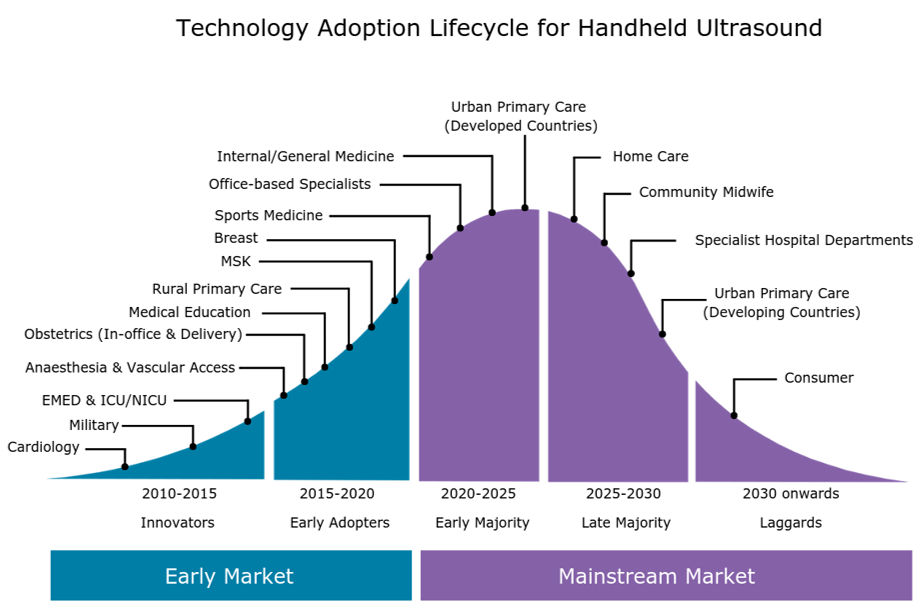
As we discussed in a previous insight ("Handheld Ultrasound Market Poised for Next Wave of Growth"), the handheld ultrasound market is growing rapidly as the latest generation of ultraportable devices gains acceptance among a diverse range of customer groups, from emergency medicine physicians and intensivists to internists, office-based specialists, and -- looking forward -- primary care physicians.
The expanding customer base of handheld systems, coupled with the increased availability of affordable handheld scanners, is forecast to boost global sales of handheld ultrasound by more than 50% in 2019. By 2023, the global market for handheld ultrasound is forecast to exceed $400 million.

5. Artificial intelligence to transform market
Artificial intelligence (AI) will have a transformative effect on the ultrasound market as AI addresses some of the key limitations associated with ultrasound; namely, the shortage of trained sonographers and the relatively steep learning curve, high operator dependency during image acquisition and interpretation, poor image quality for certain exam types, and relatively lengthy exam time compared with other modalities.
The first wave of ultrasound AI applications are entering the market and are mainly for image optimization (noise reduction) and automation of time-consuming and repetitive tasks, such as anomaly detection, image labeling, and feature quantification. However, the greatest impact of AI will be on guided ultrasound (ultrasound navigation), which will provide real-time support during image acquisition (i.e., probe placement and anatomy detection).
The first AI-enabled guided ultrasound systems are expected to be released in the second half of 2019. These systems are expected to expand the user base by making ultrasound more accessible to novice users, particularly in acute and primary care.
Thứ Ba, 18 tháng 6, 2019
Which biopsy method best detects prostate cancer?
By Wayne Forrest, AuntMinnie.com staff writer
June 18, 2019 -- The combination of ultrasound- and MRI-guided biopsy yields the best chance of detecting prostate cancer, as each method can find malignant lesions missed by the other, researchers from the University of California, Los Angeles (UCLA) reported in a study published online June 12 in JAMA Surgery.
In the three-year Prospective Assessment of Image Registration in the Diagnosis of Prostate Cancer (PAIREDCAP) study, the researchers found that using ultrasound and MRI in tandem can identify up to one-third more cancers than standard techniques.
"Our research suggests that the different biopsy methods identify different tumors," said senior author Dr. Leonard Marks, from UCLA's department of urology, in a statement. "To maximize our ability to identify prostate cancer, we need to take advantage of all the information we can. Our cancer detection rate, while using different methods in tandem, surpasses that from using either method alone."
While the clinical value of MRI-guided prostate biopsy has been proved in previous large prospective studies, some debate remains over the optimum approach with the modality. Clinicians have debated whether biopsy should focus on areas with lesions only visible on MRI or if ultrasound-guided systematic biopsy -- in which 12 biopsy cores are acquired of multiple areas of the prostate -- is sufficient.
"Answers to these questions are vital because of the importance of diagnosing prostate cancer early vis-a-vis cost-effectiveness issues," the authors wrote.
The prospective study included 300 men who were undergoing prostate biopsy for the first time: 248 consecutive subjects (mean age, 65.5 ± 7.7 years) had MRI-visible lesions, while the control population consisted of 52 men (mean age, 63.6 ± 5.9 years) with no visible lesions on MRI. Each biopsy was preceded by a 3-tesla multiparametric MRI scan (Magnetom Trio, Siemens Healthineers) with an abdominal coil within 60 days of the procedure.
The study protocol used three biopsy techniques:
- Systematic biopsy, performed with a standard handheld transrectal ultrasound-guided technique in which 12 cores were acquired, with the operator blinded to the MRI results
- Targeted cognitive fusion, in which a radiologist used MR images on a screen next to the patient to guide the urologic biopsy operator to aim an ultrasound-guided biopsy at the area of the prostate corresponding to where the lesion was seen on MRI; three biopsy cores were obtained cognitively from the index region of interest (ROI)
- Software fusion, in which researchers fused MRI and 3D ultrasound images using commercially available software (Artemis, Eigen), and an operator performed three targeted biopsies on the coregistered images
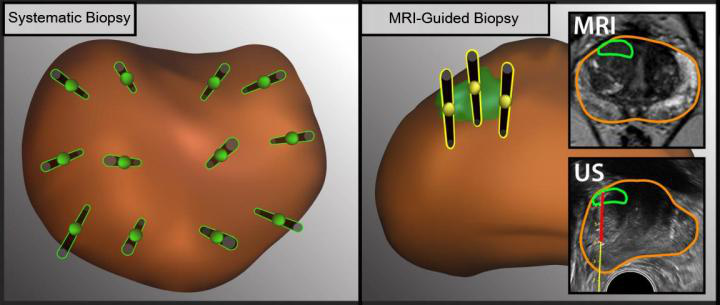
The illustration shows the difference between ultrasound- and MRI-guided methods to obtain tissue samples (black needles) from different regions in the prostate (brown oval object). MRI (right) allows doctors to detect lesions (green oval object) and take tissue samples from specific lesions. Images courtesy of UCLA Health.
The combination of methods produced the highest results, the researchers found.
| Cancer detection rate of prostate biopsy methods | |
| Biopsy method | Cancer detection rate |
| Combination of systematic, cognitive, and software fusion biopsy | 70.2% |
| Cognitive fusion or software fusion | 62.1% |
| Cognitive targeting | 46.8% |
The cancer detection rate of 70% is considerably higher than the cancer detection rate of conventional biopsy in previous studies, likely reflecting the outcomes of the MRI screening, the researchers noted. "These data thus serve to confirm the value of MRI for providing risk assessment when considering biopsy," they wrote.
Indeed, the researchers found that if only a single biopsy method was used, from 11.5% to 33.3% of cancers would have been missed, based on patient population.
Interestingly, among the 52 healthy controls, traditional ultrasound found prostate cancer in eight men (15%). This means that MRI does not identify all tumors, thus heightening the need to also incorporate traditional ultrasound-guided systematic biopsy as well, according to the researchers.
Ultrasound helps assess DVT risk after ablation
By Kate Madden Yee, AuntMinnie.com staff writerJune 18, 2019
The researchers from Stanford University also found that ultrasound helped clarify which ablation technique is safer.
"The rates of DVT decreased over time, suggesting an improvement in overall procedural safety; however, LA demonstrated a considerable decreased risk for DVT when compared to RFA," first author Dr. Nathan Itoga and colleagues wrote.
Studies have shown that both radiofrequency ablation and laser ablation are at least as successful as surgery for treating conditions such as varicose veins, and they can be performed without general anesthesia and tend to have fewer negative effects. But the rates of complications such as DVT after venous ablation procedures have been unclear, the group noted.
"Despite the relative safety of these techniques, LA and RFA may cause endovenous heat-induced thrombosis which ... may extend or propagate, leading to deep vein thrombosis," the researchers wrote. "In rare cases, LA and RFA procedures may also lead to pulmonary embolism. The overall risk for thromboembolic complication after endovenous ablation is controversial, and estimates in the literature vary greatly, from less than 1% to 18%."
The study included data from Truven Health Analytics MarketScan databases from 2007 and 2016 for a cohort of patients who underwent RFA or LA and had a follow-up duplex ultrasound scan within seven days and 30 days of the ablation procedure. Of the patient cohort, 256,999 underwent 433,286 ablations, 44.4% of which were radiofrequency and 55.6% of which were laser.
Of these patients, 1.9% had a newly diagnosed DVT within seven days of the procedure, and 3.1% had a newly diagnosed DVT within 30 days of the procedure. Factors associated with a decreased risk of DVT within 30 days included having had laser ablation, being female, and having sclerotherapy performed on the same day as the ablation; factors associated with an increased risk of DVT included a diagnosis of peripheral artery disease and undergoing stab phlebectomy.
Screening ultrasound revealed laser ablation to be the safer method, showing an 18% decrease in the incidence of DVT at 30 days (2.8%) compared to radiofrequency ablation (3.4%).
The study results demonstrate ultrasound's usefulness in tracking patients who have undergone ablation procedures for complications, according to the researchers.
"Some have suggested that postoperative evaluation of DVT is unnecessary, arguing that ultrasound overdiagnoses DVT, leading to overtreatment," Itoga and colleagues wrote. "However, if postoperative ultrasound were reserved for only those with symptoms, a considerable number of DVT would be missed."
Thứ Bảy, 15 tháng 6, 2019
Better ultrasound protocols slash trauma imaging overuse.
By Kate Madden Yee, AuntMinnie.com staff writer
June 11, 2019 -- When lower extremity duplex ultrasound screening (LEDUS) protocols for the trauma department are refined, overuse of hospital resources is reduced by more than a third -- and without negative effect on patient outcomes, according to a new study published June 5 in the Journal of Surgical Research.
The findings translate to more efficient trauma departments -- and better patient care, wrote a team led by Dr. Jennifer Baker of the University of Cincinnati in Ohio.
"Refinement of LEDUS protocols can decrease overutilization of hospital resources without compromising trauma patient outcomes," the researchers concluded.
A tool called the risk assessment profile (RAP) is typically used in the trauma center to identify patients who would most benefit from lower extremity duplex ultrasound screening. But it can lead to overuse of imaging and needs refinement, Baker's group wrote.
The researchers conducted a study for which they hypothesized that revising their hospital's LEDUS protocol so that screening ultrasound examinations were performed in patients with a RAP score ≥ 8 within 48 hours of admission would reduce the number of screenings performed -- without changing patient outcomes.
The study included 1,014 trauma patients admitted from July 2014 to June 2015 and July 2016 to June 2017. From 2014 to 2015, patients with a RAP score ≥ 5 had weekly LEDUS examinations starting on the fourth hospital day, while from 2016 to 2017, the protocol changed to screening patients with a RAP score ≥ 8 by the second hospital day. Both protocols included screening with weekly ultrasound after the first examination. Baker's team gathered data on demographics, injury characteristics, LEDUS exam findings, and venous thromboembolism incidences.
The group found that from 2014 to 2015, 602 patients underwent LEDUS exams, but from 2016 to 2017, only 412 patients did: a 32% drop. Significantly, the team noted no difference in the number of patients diagnosed with deep vein thrombosis (DVT) or pulmonary embolism between the two protocols; in fact, DVT was often identified in the first LEDUS exam in both year groups.
Regarding those patients who received a DVT diagnosis on first LEDUS exam, the group also found the following:
- These patients had significantly higher RAP scores than those who did not have a DVT diagnosis (12 versus 10).
- The time to their first LEDUS exam was shorter (one day versus three days).
- The DVT diagnosis was made more quickly (two versus four days).
A simple change to protocol can make a big difference without harming patients, according to the researchers.
"[This protocol change caused] no significant difference ... in the number of patients diagnosed with DVT or pulmonary embolism," they concluded.
Thứ Bảy, 8 tháng 6, 2019
Thứ Năm, 6 tháng 6, 2019
Ultrasound shows Heart disease Risk from Psoriasis.
June 6, 2019 -- Ultrasound imaging of the carotid arteries can help identify patients with psoriasis and psoriatic arthritis who are at increased risk for heart disease by revealing the extent of clogging in patients' arteries, according to a new study published online June 5 in Arthritis & Rheumatology.
The results show that combining ultrasound imaging data with traditional cardiovascular risk factors -- as measured by, for example, the Framingham risk score -- could identify which patients with psoriatic disease may benefit from more intensive heart-protective therapies, wrote lead author Dr. Curtis Sobchak, of the University of Toronto, and colleagues.
"Ultrasound is widely used in rheumatology settings as a point of care to detect joint inflammation. Our study suggests that ultrasound can also be used to identify patients that are at high cardiovascular risk who may be missed by the conventional methods such as the Framingham risk score," senior author Dr. Lihi Eder, PhD, said in a statement released by the journal. "This will allow early intervention, such as initiation of lipid lowering therapy, which will ultimately lower the risk of developing cardiovascular events."
Sobchack and colleagues evaluated whether carotid ultrasound could predict incident cardiovascular events in patients with psoriatic disease and whether using ultrasound imaging data would improve the performance of the Framingham risk score for cardiovascular risk prediction.
The study included 559 patients with psoriatic disease. Of these, 23 had experienced cardiovascular events that suggested heart disease. Patients underwent ultrasound of the carotid arteries between December 2009 and December 2015; the researchers then assessed the extent of atherosclerosis by measuring carotid intima media thickness and total plaque area, evaluating the patients' risk of experiencing further cardiovascular events using a hazard ratio (HR) model (with base HR equal to 1).
The team found that the rate at which patients experienced their first cardiovascular event during the study period was 1.11 events per 100 patient years. The group also found the following factors predicted incident cardiovascular events after controlling for the Framingham risk score:
| Factors on carotid ultrasound that predict cardiovascular events | |
| Hazard ratio | |
| Total plaque area | 3.74 |
| High total plaque area category | 3.25 |
| Mean carotid intima media thickness | 1.21 |
| Max carotid intima media thickness | 1.11 |
Since carotid atherosclerosis is associated with an increased risk of developing future heart disease -- and since patients with psoriatic disease are known to be at increased risk of heart disease -- using ultrasound-generated vascular imaging data with information on traditional cardiovascular risk factors could improve the accuracy of cardiovascular risk assessment in these patients, according to the group. And ultrasound has many benefits when compared with other imaging modalities.
"The advantage of ultrasound over other modalities for vascular imaging includes lack of radiation, low cost of the examination, and its widespread use in rheumatology for joint evaluation," the team concluded. "Thus, this assessment could potentially be performed 'at the bedside' during consultation to provide immediate valuable information to complement clinical data from history, physical examination, and laboratory data."
Đăng ký:
Nhận xét
(
Atom
)










