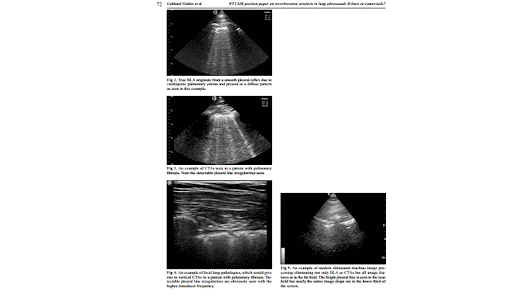
The analysis of vertical reverberation artefacts is an essential component of the differential diagnosis in pulmonary ultrasound. Traditionally, they are often, but not exclusively, called B-line artefacts (BLA) and/or comet tail artefacts (CTA), but this view is misleading.
In this position paper we clarify the terminology and relation of the two lung reverberation artefacts BLA and CTA to specifc clinical scenarios. BLA are defned by a normal pleura line and are a typical hallmark of cardiogenic pulmonary edema after exclusion of certain pathologies including pneumonia or lung contusion, whereas CTAs show an irregular pleura line representing a variety of parenchymal lung diseases. The dual approach using low frequency transducers to determine BLA and high frequency transducer to determine the pleural surface is recommended.
Keywords: lung ultrasound; artefact; B-lines; comet tails; guidelines; misdiagnosis
The transducer should be positioned such that the emenating ultrasound beam perpendicularly intersects
the surface of the lung to maximize likelihood of seeing all BLA and CLA as well as A line artifacts (fig 1).
A recent study highlighted the potentially detrimental effects of placing the focal zone below the pleural line,using spatial compounding, higher frequency and tissue harmonics [14]. Once machine settings and transducer orientation have been optimized, we suggest that two most important and distinct vertical lung artefacts should be differentiated: BLA and CTA. While true BLA (fig 2) originate from a smooth pleural reflex due to cardiogenic pulmonary edema and present in a diffuse pattern, CTAs are seen in many lung disorders with irregular and fragmented pleural reflexes and can be focal or diffuse (fig 3).
Hence, the initial step should be to determine if there is evidence for diffuse pulmonary disease or defned focal or localized pathology. Focal lung pathologies by defnition should display vertical artifacts that are consistent with CTAs (fig 4).
Diffusely distributed vertical reverberation artefacts can be divided into two groups: with or without detectable pleural line irregularities and with stable or distally widening width:
1. The reverberation artefact (evaluated by low frequency transducer <5 MHz without interfering presets) is called BLA if arising from a smooth pleural line (evaluated by high frequency transducer ≥10 MHz). The BLA arises from edema within the interstitium, is well defned with stable width, hyperechoic and extending indefnitely (the entire depth, at least 10 cm), erasing A-lines and moving with lung sliding. It is important to realize that many modern ultrasound machines have post-processing and other features which will eliminate not only BLA but essentially all discernable image detail near the bottom of the screen at greater depths (fig 5).
The differentiation of BLA from CTA is also dependent on the technical adjustments of several external factors, including the type of ultrasound machine, transducers and probe frequencies [6].
through integration of ultrasound data with clinical presentation) in the emergency setting is crucial for the correct management of the patient. The differentiation between ultrasonographic BLA and CTA, using two types (high and low frequency) of transducers allows accurate differentiation between pulmonary edema and other cause of diffuse pulmonary pathology. Both can lead to acute respiratory failure but may require different clinical management. Localized pulmonary diseases representing with CTA are distinguished. Mixed forms of diffuse,but also diffuse and focal lung diseases have to be considered.