Nhồi
máu mạc nối lớn là nguyên nhân hiếm thấy của bụng cấp tính.
Biểu
hiện đau bụng bên P có thể gây chẩn đoán nhầm nhồi máu mạc nối lớn với viêm túi mật hay viêm ruột thừa; do đó
cần chẩn đoán hình ảnh chính xác và để
tránh mổ bụng hay điều trị kháng sinh không cần thiết.
Nhồi
máu mạc nối lớn ít gặp ở bệnh nhi (khoảng 15% số ca).
Nhồi
máu mạc nối lớn ít gặp hơn nhồi máu ruột non và ruột già vì mạc nối lớn được
tưới máu phong phú nhờ tuần hoàn bên.
Nguyên
nhân của nhồi máu mạc nối lớn không do xoắn thường gặp nhất là suy tuần hoàn
tĩnh mạch do chấn thương hoặc huyết khối tĩnh mạch mạc nối.
Các
yếu tố có xu hướng thiên về nhồi máu mạc nối lớn gồm béo phì, hoạt động gắng
sức, suy tim sung huyết, dùng digitalis, mới phẫu thuật bụng và chấn thương
bụng.
FURTHER READING:
Omental infarction: sonographic and CT findings, A. Hollerweger, P. Macheiner (2002, Mar 19).
Male, 35 year(s)
Clinical History
A patient with acute right lower quadrant abdominal pain.
Imaging Findings
The patient presented with an 18-hour history of local tenderness in the right lower abdomen. No vomiting, nausea, or fever was present. He was admitted with suspected acute appendicitis and abdominal sonography and CT examinations were performed.
Discussion
Omental infarction is an acute abdominal condition, which is often clinically misdiagnosed as acute appendicitis (1, 2). Its most common localisation, in the right mid or lower abdomen, has been explained as a congenital vascular anomaly, but segmental infarction can be localised anywhere in the omentum. Omental infarction is a relatively rare condition and may occur at any age. Approximately 15% of patients are children (3).
Patients usually present with acute or subacute abdominal pain and localised tenderness; laboratory parameters are within the normal range or show slight elevation of white blood cell count or sedimentation rate. Vomiting and nausea are rare (1, 2).
Sonography typically shows an ovoid, non-compressible, moderately hyperechoic mass at the point of maximum tenderness (1, 2, 4, 5). The mass may be surrounded by a hypoechoic rim and is frequently adherent to the parietal peritoneum of the abdominal wall. On colour Doppler sonography vascularisation is not visible in the infarcted omentum, but adjacent tissue shows moderately increased colour flow due to the inflammatory reaction.
CT scans show a corresponding fatty lesion with hyperattenuating streaks (1, 2, 5). The parietal peritoneum is often thickened, whereas the bowel wall appears normal.
Follow-up examinations show a slow decrease in lesion size and disappearance of the lesion over a period of 1–2 months.
In cases of segmental omentum infarction, both sonography and CT show characteristic features that enable the correct diagnosis. Clinical symptoms gradually disappear when treated with analgesics and, with appropriate diagnosis, unnecessary surgery can be avoided.
References
1. Puylaert JB. Right-sided segmental infarction of the omentum: clinical, US, and CT findings.
Radiology. 1992 Oct;185(1):169-72..
2.
van Breda Vriesman AC, Lohle PN, Coerkamp EG, Puylaert JB. Infarction
of omentum and epiploic appendage: diagnosis, epidemiology and natural
history.
Eur Radiol. 1999;9(9):1886-92..
3. Schlesinger AE, Dorfman SR, Braverman RM. Sonographic appearance of omental infarction in children.
Pediatr Radiol. 1999 Aug;29(8):598-601..
4. Puylaert JB. Ultrasound of acute GI tract conditions. Eur Radiol. 2001;11(10):1867-77..
5. Hollerweger A, Rettenbacher T, Macheiner P, Gritzmann N. Spontaneous fatty tissue necrosis of the omentum majus and epiploic appendices: clinical, ultrasonic and CT findings. Rofo Fortschr Geb Rontgenstr Neuen Bildgeb Verfahr. 1996 Dec;165(6):529-34..
Acute omental infarction
Norbert Gritzmann, Gruppenpraxis Radiologie Vienna Austria
Acute omental infarction most commonly manifests with acute lower quadrant pain, with the most frequent site in the right lower quadrant; acute appendicitis is the main clinical differential diagnosis. This is in contrast with another condition, acute epiploic appendagitis, which is most commonly adjacent to the sigmoid colon and presents with left lower quadrant pain. It is important to correctly diagnose both acute epiploic appendagitis and acute omental infarction on ultrasound as both these conditions may be mistaken for an "acute abdomen”, and this may lead to unnecessary surgery.
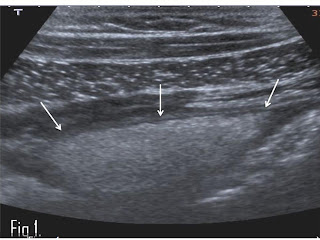
The ultrasound features of acute omental infarction include a well-circumscribed triangular or oval heterogeneous non compressible fatty mass with an echogenic alteration of the fat between the anterior abdominal wall and the transverse or ascending colon (Figure 1). The echogenic area of infarction may contain focal areas of hypo-echogenicity as well. Often this pseudo-tumour is fixed to the abdominal wall, readily identified during real-time ultrasound examination. With acute appendicitis a round non compressible tubular ending structure with a diameter of more than 6mm is usually identified on ultrasound, easily allowing differentiation from the echogenic mass of acute omental infarction seen on an ultrasound examination. With diverticulitis of the ascending colon an echogenic "out-pouching” of the colon with alteration of the surrounding fat is visualized on ultrasound.
Figure 1:A transverse view on ultrasound of the right lower quadrant in a 22 year old male patient with severe pain in this area. A 4 cm echogenic lesion is fixed to the abdominal wall (arrows). No movement of the lesion in regard to the hypo-echogenic abdominal wall muscles was seen during real time scanning.
The ultrasound pattern of acute omental infarction can be very similar to acute epiploic appendagitis, often needing a CT examination to confirm the suspicions raised on the ultrasound examination (Figure 2).
Figure 2:An axial CT image of the lower abdomen demonstrating fat stranding adjacent to the ascending colon (arrows).
As ultrasound becomes increasingly used for the evaluation of acute abdomen, recognition of these conditions will allow appropriate management of acute abdominal pain and may help to prevent unnecessary surgery.
References
* Puylaert JB. Right-sided segmental infarction of the omentum: clinical, US, and CT findings. Radiology 1992;185:169–172.
* Hollerweger A, Macheiner P, Rettenbacher T, Gritzmann N. Primary epiploic appendagitis: sonographic findings with CT correlation. J Clin Ultrasound. 2002;30:481-95.
* Baldisserotto M, Maffazzoni DR, Dora MD. Omental Infarction in Children: Color Doppler Sonography Correlated with Surgery and Pathology Findings. AJR 2005;184:156–162.
Posted : EFSUMB Admin - Tue, Nov 8, 2011 8:44 PM.


Không có nhận xét nào :
Đăng nhận xét