Nhận thư mời tham dự CME về Siêu âm đàn hồi ARFI ngày 04-7 tąi Trung tâm MEDIC Hòa Hảo, số 254, Hòa Hảo, Q 10:
Phòng Siêu âm Lầu 1 Khu A.
Hạn trước 1-7-2015
Xác nhận tham dự với
Ms Ngô thị Tâm (Siemens) : Mob: 01669262002
Đã tổ chức thành công với 162 bác sĩ siêu âm từ Huế, Nha trang đến Cà mau và các tỉnh phía nam và thành phố HCM tham dự.
Bs Nguyễn Thiện Hùng, Phòng Siêu âm Medic: Mob: 0918188372
email : medichh@yahoo.com
Tổng số lượt xem trang
Thứ Ba, 23 tháng 6, 2015
Thứ Bảy, 20 tháng 6, 2015
Dedicated Training Program for Shoulder Sonography
Sonography is a commonly used diagnostic imaging modality for evaluation of rotator cuff tears, in part
because this modality has lower cost and accuracy comparable to that of magnetic
resonance imaging (MRI).1–7 In the United States, the use of musculoskeletal
sonography increased by 316% between 2000 and 2009; this increase was driven
primarily by nonradiologists8 and continued the utilization growth trend of the
previous decade.9
However, in the United States, unlike in Europe and Asia, sonography is not
considered a first-line imaging modality for shoulder pain.7,10 In addition,
the usefulness of shoulder sonography is widely considered to be operator
dependent, with the radiologist’s experience being the primary factor in this
imaging modality’s effectiveness.11–13
Several studies have found little agreement in sonographic results between less- and more-experienced operators, even when the operators were evaluating full-thickness tears.13,14 Other studies have found good to excellent reliability of sonography for the diagnosis of full-thickness rotator cuff tears but less satisfactory detection sensitivity for partialthickness tears.1,4,11,14 In a meta-analysis of 65 studies, de Jesus et al2 found no differences between MRI and sonography in sensitivity or specificity for detection of full or partial rotator cuff tears.
Given these variable results, many non-European radiologists may believe that musculoskeletal sonography is a difficult technique to learn and implement and may thusexclude it from clinical practice in patients with shoulder pain. However, with the current economic climate, we wished to challenge both this hypothesis and the current dependency on MRI for the diagnosis of shoulder disorders. In this study, we assessed the effect of implementing an open-ended, comprehensive training program on the diagnostic accuracy of shoulder sonographic interpretation in a clinical practice.
Several studies have found little agreement in sonographic results between less- and more-experienced operators, even when the operators were evaluating full-thickness tears.13,14 Other studies have found good to excellent reliability of sonography for the diagnosis of full-thickness rotator cuff tears but less satisfactory detection sensitivity for partialthickness tears.1,4,11,14 In a meta-analysis of 65 studies, de Jesus et al2 found no differences between MRI and sonography in sensitivity or specificity for detection of full or partial rotator cuff tears.
Given these variable results, many non-European radiologists may believe that musculoskeletal sonography is a difficult technique to learn and implement and may thusexclude it from clinical practice in patients with shoulder pain. However, with the current economic climate, we wished to challenge both this hypothesis and the current dependency on MRI for the diagnosis of shoulder disorders. In this study, we assessed the effect of implementing an open-ended, comprehensive training program on the diagnostic accuracy of shoulder sonographic interpretation in a clinical practice.
Discussion
Shoulder sonography is becoming increasingly popular for the diagnosis of rotator cuff tears due in part to its lower cost, accessibility, and results that are similar to those obtained with MRI.1–4 However, sonography is not the first-line imaging test for shoulder pain in the United States, likely because operator experience is thought to contribute to variable diagnostic accuracy and reproducibility.2,11–14,16,17 This lack of preference for shoulder sonography is the case despite the American College of Radiology appropriateness criteria rating of sonography as 8 or 9 (usually appropriate) for patients older than 35 years with shoulder pain and suspected rotator cuff tears/impingement.16 In addition, the American College of Radiology appropriateness criteria rate sonography as 5 (maybe appropriate) should MRI (9, usually appropriate) be contraindicated for patients with ersistent pain.
In contrast, the American College of Radiology appropriateness score for sonography increases to 8 of 9 (usually appropriate) for evaluation of the postoperative cuff or in patients older than 35 years with suspected impingement.
In one study, the interobserver concordance for the diagnosis of full- and partial-thickness rotator cuff tears on independent examinations was found to be high (92%) between 2 operators with more than 5 years of shoulder sonography experience.16 Another study found that agreement between an experienced musculoskeletal radiologist and a general radiologist with no experience in shoulder sonography was 98% for full-thickness rotator cuff tears and 90% for partial-thickness tears.11 These studies demonstrated good inter-rater measurement reproducibility; however, in the second study, the sensitivity, specificity, and accuracy for the detection of full-thickness rotator cuff tears relative to surgery as a reference standard were 3% to 4% lower for the general radiologist than for the experienced musculoskeletal radiologist.11 Another study evaluated the learning curves for 2 orthopedic surgeons using office-based sonographic examinations to detect full-thickness supraspinatus tears previously diagnosed with MRI.12 In this study, at least 100 shoulder sonographic examinations were required to enable each surgeon to detect full-thickness tears, with diagnostic accuracy of 67 of 72 (93%) and 92 of 95 (97%), respectively, in the second round of 100 examinations. The variability in reported operator accuracy for rotator cuff disorders other than for full-thickness tears2,11–14,16,17 may have led to a lack of confidence in sonographically based diagnoses. Nevertheless, agreement and accuracy for the diagnosis of full-thickness tears are high.1,2,11,13,14
....
Shoulder sonography is becoming increasingly popular for the diagnosis of rotator cuff tears due in part to its lower cost, accessibility, and results that are similar to those obtained with MRI.1–4 However, sonography is not the first-line imaging test for shoulder pain in the United States, likely because operator experience is thought to contribute to variable diagnostic accuracy and reproducibility.2,11–14,16,17 This lack of preference for shoulder sonography is the case despite the American College of Radiology appropriateness criteria rating of sonography as 8 or 9 (usually appropriate) for patients older than 35 years with shoulder pain and suspected rotator cuff tears/impingement.16 In addition, the American College of Radiology appropriateness criteria rate sonography as 5 (maybe appropriate) should MRI (9, usually appropriate) be contraindicated for patients with ersistent pain.
In contrast, the American College of Radiology appropriateness score for sonography increases to 8 of 9 (usually appropriate) for evaluation of the postoperative cuff or in patients older than 35 years with suspected impingement.
In one study, the interobserver concordance for the diagnosis of full- and partial-thickness rotator cuff tears on independent examinations was found to be high (92%) between 2 operators with more than 5 years of shoulder sonography experience.16 Another study found that agreement between an experienced musculoskeletal radiologist and a general radiologist with no experience in shoulder sonography was 98% for full-thickness rotator cuff tears and 90% for partial-thickness tears.11 These studies demonstrated good inter-rater measurement reproducibility; however, in the second study, the sensitivity, specificity, and accuracy for the detection of full-thickness rotator cuff tears relative to surgery as a reference standard were 3% to 4% lower for the general radiologist than for the experienced musculoskeletal radiologist.11 Another study evaluated the learning curves for 2 orthopedic surgeons using office-based sonographic examinations to detect full-thickness supraspinatus tears previously diagnosed with MRI.12 In this study, at least 100 shoulder sonographic examinations were required to enable each surgeon to detect full-thickness tears, with diagnostic accuracy of 67 of 72 (93%) and 92 of 95 (97%), respectively, in the second round of 100 examinations. The variability in reported operator accuracy for rotator cuff disorders other than for full-thickness tears2,11–14,16,17 may have led to a lack of confidence in sonographically based diagnoses. Nevertheless, agreement and accuracy for the diagnosis of full-thickness tears are high.1,2,11,13,14
....
Because the study was retrospective,
varying standards of patient care may have been used, as well as
nonstandardized radiology and surgical
report language. Standardization of this report nomenclature with prospectively
defined terminology would decrease reporting variability and aid in the comparison
of results. In addition, the range of musculoskeletal sonography experience may
have increased the variability of the study results. We did not separate out the
examinations interpreted by the most experienced sonographer because we believe
that the benefits of acquisition and interpretation standardization as well as
feedback based on surgical correlation also improved the accuracy of this radiologist’s
sonographic work. Finally, because of the retrospective nature of this study,
the patient population was inhomogeneous with regard to referral patterns,
symptoms, and the distribution of tendon tears across groups.
The results of this retrospective study demonstrate that introducing musculoskeletal sonography into a new clinical practice is not only feasible but can be accomplished with high diagnostic accuracy. The use of musculoskeletal sonography may enable a decrease in health care costs by substitution of a diagnostic musculoskeletal sonographic examination for a shoulder MRI examination.7 The use of sonography as a first-line diagnostic imaging modality for shoulder pain is warranted, as evidenced by the European guidelines.10
Furthermore, based on the findings of this study, we believe that the implementation of a systematic quality improvement program, including acquisition protocol standardization and a comprehensive, ongoing educational program for all team members, can improve the diagnostic performance of all aspects of musculoskeletal sonography, not only sonography limited to rotator cuff injuries.
Although operator experience cannot be ruled out as a factor in sonographic interpretation, this study demonstrates that education provided to a group of operators with a wide variety of experience increases the diagnostic sensitivity and accuracy of sonography for detecting full-thickness supraspinatus and infraspinatus tendon tears.
In conclusion, implementation of formal, ongoing training that embraces all team members, standardizes acquisition and interpretation protocols, and provides a forum for continuous quality improvement raises the diagnostic accuracy and sensitivity of shoulder sonography for rotator cuff injuries. Our work supports the potential of musculoskeletal sonography as a first-line imaging modality for shoulder pain when rotator cuff disorders are suspected.7,10 By implementing an open-ended training program for the entire care team, musculoskeletal sonography can be easily and successfully introduced into a new clinical practice with high diagnostic accuracy.
The results of this retrospective study demonstrate that introducing musculoskeletal sonography into a new clinical practice is not only feasible but can be accomplished with high diagnostic accuracy. The use of musculoskeletal sonography may enable a decrease in health care costs by substitution of a diagnostic musculoskeletal sonographic examination for a shoulder MRI examination.7 The use of sonography as a first-line diagnostic imaging modality for shoulder pain is warranted, as evidenced by the European guidelines.10
Furthermore, based on the findings of this study, we believe that the implementation of a systematic quality improvement program, including acquisition protocol standardization and a comprehensive, ongoing educational program for all team members, can improve the diagnostic performance of all aspects of musculoskeletal sonography, not only sonography limited to rotator cuff injuries.
Although operator experience cannot be ruled out as a factor in sonographic interpretation, this study demonstrates that education provided to a group of operators with a wide variety of experience increases the diagnostic sensitivity and accuracy of sonography for detecting full-thickness supraspinatus and infraspinatus tendon tears.
In conclusion, implementation of formal, ongoing training that embraces all team members, standardizes acquisition and interpretation protocols, and provides a forum for continuous quality improvement raises the diagnostic accuracy and sensitivity of shoulder sonography for rotator cuff injuries. Our work supports the potential of musculoskeletal sonography as a first-line imaging modality for shoulder pain when rotator cuff disorders are suspected.7,10 By implementing an open-ended training program for the entire care team, musculoskeletal sonography can be easily and successfully introduced into a new clinical practice with high diagnostic accuracy.
Dedicated Training Program for Shoulder
Sonography, Patricia B. Delzell, MD, Alex Boyle, Erika
Schneider, PhD, J Ultrasound Med 2015; 34:1037–1042
Thứ Sáu, 19 tháng 6, 2015
Thứ Năm, 11 tháng 6, 2015
Thứ Tư, 10 tháng 6, 2015
SIÊU ÂM 5D LÀ GÌ ? Dr Jasmine Thanh Xuân. Medic Medical Center
Cty Samsung Korea vừa đưa ra khái niệm siêu âm 5 chiều (SA 5D) trên máy W80A chuyên SA sản phụ khoa. Trước đây, SA 3D, 4D chỉ dừng lại ở khảo sát hình thái ngoài của thai nhi mà không thấy được các cấu trúc bên trong khối này. SA 5D, thêm một chiều nữa là chiều chẩn đoán ( Diagnostic Dimension). Cấu trúc hình khối sẽ được tự động phân tích thành loạt hình thường quy trong SA chẩn đoán thai, tự động đo đạc chỉ bằng một nút bấm trên bàn phím. Các ứng dụng hiện có : 5D tim thai ( 5D fetal heart), 5D hệ TKTW ( 5D CNS), 5D hệ xương dài (5D LB), 5D đo da gáy ( 5D NT) và 5D trong khảo sát nang noãn ( 5D Follicle).
- 5D fetal heart: trình bày cùng lúc 9 mặt cắt cơ bản trong khảo sát tim, trong cùng một chu chuyển tim, cho phép quan sát về hình thể ( morphology) và cử động các lá van ( movement) rất sinh động, tự động đánh dấu các buồng tim, các mạch máu lớn. Đòi hỏi BS siêu âm thai phải biết rõ về bệnh học tim bẩm sinh thai nhi.
- 5D CNS: trình bày cùng lúc 3 mặt cắt cơ bản qua não thai nhi ( mặt cắt qua đồi thị, qua não thất bên và tiểu não- hố sau), hiển thị ngay lập tức 6 thông số thường quy: BPD, OFD, HC, NÃO THẤT BÊN, TIỂU NÃO , HỐ SAU chỉ với một nút bấm trên bàn phím.
- Các ứng dụng đo đạc ít giá trị hơn là đo hệ xương dài ( 5D LB), đo da gáy tự động ( 5D NT).
- Ngoài ứng dụng khảo sát thai, còn một ứng dụng trong khảo sát nang noãn buồng trứng
( 5D Follicle). Phần mềm tự động phát hiện, đo đạc thể tích và kích thước từng nang noãn
( dài x rộng x cao), có thể đo cùng lúc 20 nang noãn và trình bày chi tiết trong report của máy chỉ với một nút bấm trên bàn phím, giúp tiết kiệm thời gian, hữu ích trong IVF.
Thứ Hai, 8 tháng 6, 2015
ONE or more ELASTOGRAPHIC METHODS for LIVER FIBROSIS ASSESSMENT
NOTA:
Ultrasound based-elastographic techniques
are classified in: strain techniques and shear wave elastography techniques.
Three types of elastographic techniques are included in the last category:
Transient Elastography (TE), point Shear Wave Elastography (pSWE) and shear wave elastography
(SWE) imaging (including 2D-SWE and 3D-SWE).
In
the pSWE category two techniques are included: Acoustic Radiation Force Impulse
(ARFI) elastography and ElastPQ which look very similar, but there are some
differences regarding their physical principles.
Regarding ARFI elastography
technique, the ultrasound probe produces an acoustic “push” pulse that
generates shear-waves which propagate into the tissue. Their speed, measured in
meters/second (m/s), is displayed on the screen and reflects the underlying
tissue stiffness (influenced mainly by liver fibrosis), the propagation speed increasing
with tissue stiffness. Using image-based localization and a proprietary
implementation of ARFI technology, shear wave speed may be quantified, in a
precise anatomical region, focused on a region of interest, with a predefined
size, provided by the system.
Very few information are available regarding the physical principles of ElastPQ
technique. According to the data provided by the manufacturer in the application for approval submitted
to the US Food and Drug Administration (FDA), ElastPQ system is relatively
similar with Aixplorer system® (SuperSonic Imagine S.A., Aix-enProvence,
France), which is a 2D-SWE. ElastPQ system generates an electronic voltage
pulse, which is transmitted to the transducer. In the transducer, a piezo
electric array converts the electronic pulse into an ultrasonic pressure wave.
When coupled to the body, the pressure wave transmits through body tissues. The
Doppler functions of the system process the Doppler shift frequencies from the echoes
of moving targets, such as blood, to detect and graphically display the Doppler
shift of these tissues as flow. The Doppler mode creates waves in soft tissues
and estimates the tissue stiffness by determining the speed at which these
shear waves travel.
The usefulness of ARFI elastography for non-invasive assessment of liver fibrosis was demonstrated in the last 2-3 years in international multicenter studies [5] and meta-analyses [6-8], but ElastPQ is a newly developed technique and few data are available.
The usefulness of ARFI elastography for non-invasive assessment of liver fibrosis was demonstrated in the last 2-3 years in international multicenter studies [5] and meta-analyses [6-8], but ElastPQ is a newly developed technique and few data are available.
2D –Shear Wave Elastography (2D-SWE):
The evaluation of liver stiffness [LS ] by 2D–SWE was
performed with an Aixplorer® ultrasound system (SuperSonic Imagine S.A.,
Aix-en-Provence, France), using a SC6-1 convex probe. By this technique a
quantitative elasticity map of the medium was obtained. This map is required to
image the propagation of the shear-wave and to measure its velocity. Because
the shear waves generated into the tissue by the acoustic pulse propagate at a
few meters per second, a frame rate of several kilohertz is needed to image
them. This is not possible using conventional ultrasound scanners (they usually
reach a frame rate of approximately 50 Hz). For this reason, an ultrafast,
ultrasonic scanner is required, able to remotely generate the mechanical shear
wave, by focusing ultrasound at a given location, and image the medium during
the wave propagation at a very high-frame rate (up to 6000 images/s). 2D-SWE
technique allows the acquisition of echographic images at a pulse repetition
that can reach 6000 Hz. The results of LS measurement may be displayed in units
of shear wave velocity (meters/second) or converted into units of Young’s modulus
(kPa), similar with TE.
Thứ Sáu, 29 tháng 5, 2015
Thứ Tư, 27 tháng 5, 2015
USING HEPATORENAL INDEX for HEPATIC STEATOSIS
Hepatic steatosis and nonalcoholic fatty liver disease are the most
prevalent forms of liver disease worldwide, ranging as high as 10% to 24% in
certain countries.1 Steatosis is observed
in a staggering 75% of obese people, 35% of whom will progress to nonalcoholic
fatty liver disease2 despite no evidence
of excessive alcohol consumption. Steatosis, the single most common cause of abnormal
liver function test results in the United States,1 is associated with
myriad causes, including chronic hepatitis, alcohol, drugs, toxins, obesity, and diabetes.3 Steatosis is
histopathologically defined as the intracytoplasmic accumulation of triglycerides
in a liver cell.4 Excess lipid
accumulates in vesicles (vacuoles). When vesicles are large enough to distort
the nucleus, the condition is known as macrovesicular steatosis; otherwise, the
condition is known as microvesicular steatosis. Macrovesicular steatosis is the
most common form, and the diagnosis is made whenthe percentage of hepatocytes
containing lipid droplets exceeds 5% on a continuous scale from 0 to 100.5 Indeed, cirrhosis remains the most important risk factor in the development of hepatocellular carcinoma, although hepatocellular
carcinoma can arise without cirrhosis, raising the possibility of a direct
carcinogenic link secondary to nonalcoholic fatty liver disease and steatosis.6
In addition, not only are steatotic livers associated with a greater risk of allograft dysfunction in liver transplantation, but in the foreseeable future, steatosis and its cousin nonalcoholic steatohepatitis will surpass the current primary indications for liver transplantation (eg, chronic hepatitis C infection and alcohol-related cirrhosis).7 In addition, fatty liver has been shown to negatively affect graft survival,
which is of serious concern, since steatosis affects about 25% of donors for liver transplantation and 20% of patients undergoing liver resection.
In addition, not only are steatotic livers associated with a greater risk of allograft dysfunction in liver transplantation, but in the foreseeable future, steatosis and its cousin nonalcoholic steatohepatitis will surpass the current primary indications for liver transplantation (eg, chronic hepatitis C infection and alcohol-related cirrhosis).7 In addition, fatty liver has been shown to negatively affect graft survival,
which is of serious concern, since steatosis affects about 25% of donors for liver transplantation and 20% of patients undergoing liver resection.
Sonography has been used to quantify steatosis. Webb et al9 and, more recently, Marshall et al10 used sonography, specifically
the hepatorenal index, as a quantitative tool to produce a reliable and
effective method for evaluating and screening patients with steatosis.
Initially, Webb et al9 found a correlation
between the hepatorenal index and biopsy results sufficient to quantify hepatic
steatosis exceeding 5%, but the method used a single scanner and proprietary
software, so this approach is not available to all radiologists. Marshall et al10 built on that study
by using selection criteria not based on imaging, making the results more
applicable to the general population. More important, they placed regions of
interest (ROIs) at the same sonographic depth and within the focal zone for
determining the hepatorenal index, eliminating changes in image characteristics
caused by gain adjustments to decrease external influences and produce a more
reliable hepatorenal index.10
However,
the technique used by Marshall et al relied on freeware from the National
Institutes of Health (Bethesda, MA) called ImageJ. This software required
converting images on a picture archiving and communication system (PACS) into
JPEG images, as well as downloading outside software, making the process of
hepatorenal index calculation cumbersome and time-consuming. Such an approach is
not easily adopted by radiologists.
Chủ Nhật, 24 tháng 5, 2015
Chủ Nhật, 19 tháng 4, 2015
ElastoScan ứng dụng cho sản phụ khoa
ElastoScan
TM ứng dụng cho sản phụ khoa – Khả năng phát hiện thay đổi độ đặc của cổ tử
cung trong suốt thời kì mang thai.
Trong một số trường hợp, có thể đánh giá tình trạng cổ tử cung bằng xúc chẩn. Cervix ElastoScan TM có thể đánh giá chính xác hơn tình trạng cổ tử cung.
Trong một số trường hợp, có thể đánh giá tình trạng cổ tử cung bằng xúc chẩn. Cervix ElastoScan TM có thể đánh giá chính xác hơn tình trạng cổ tử cung.
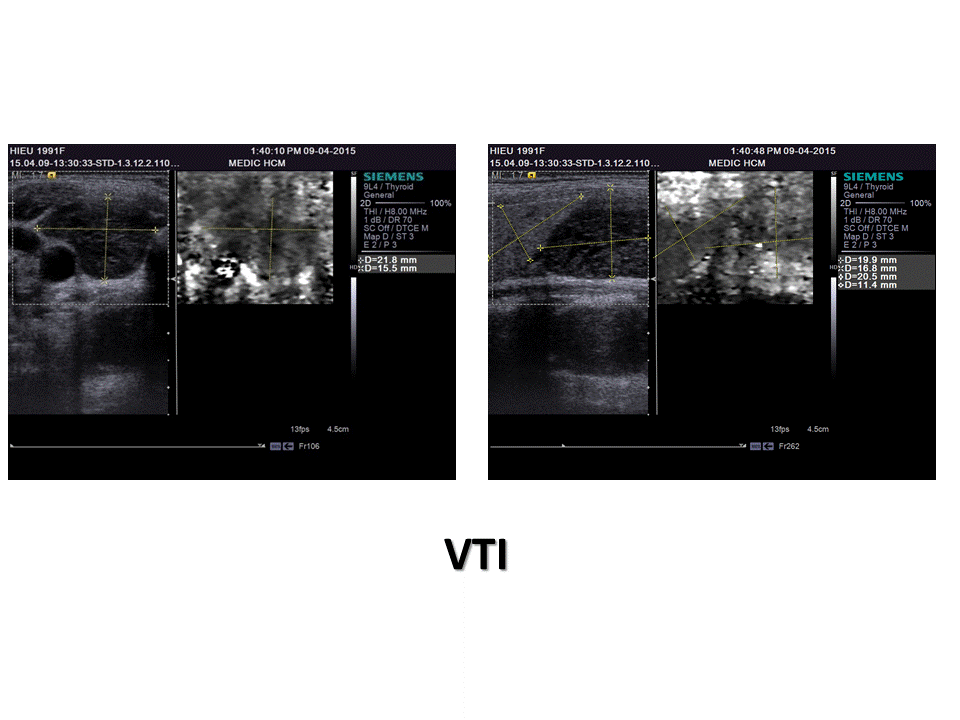
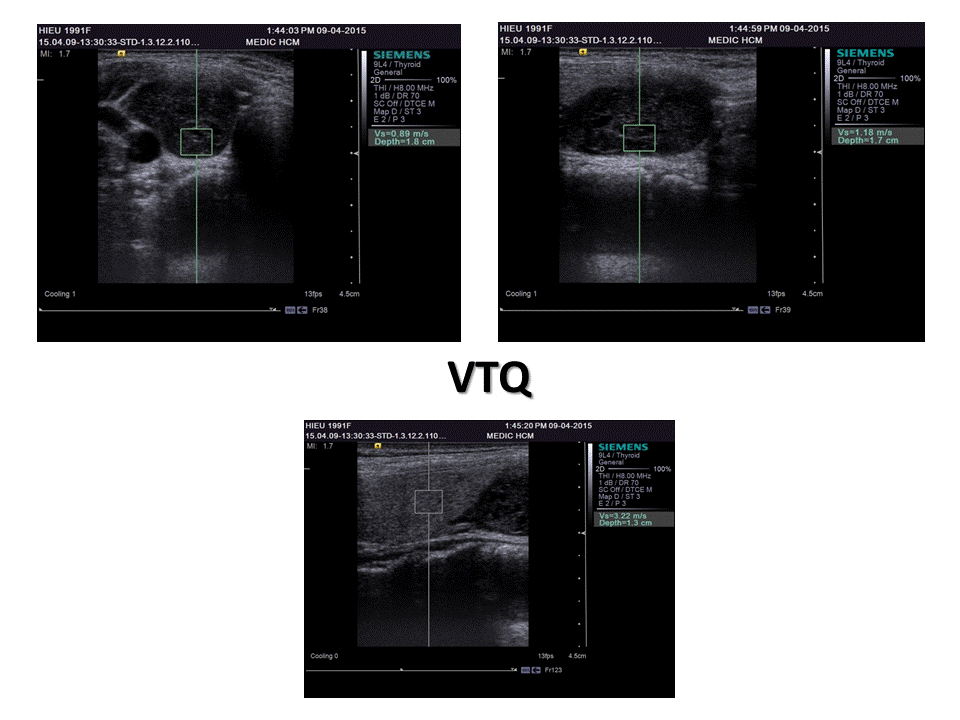
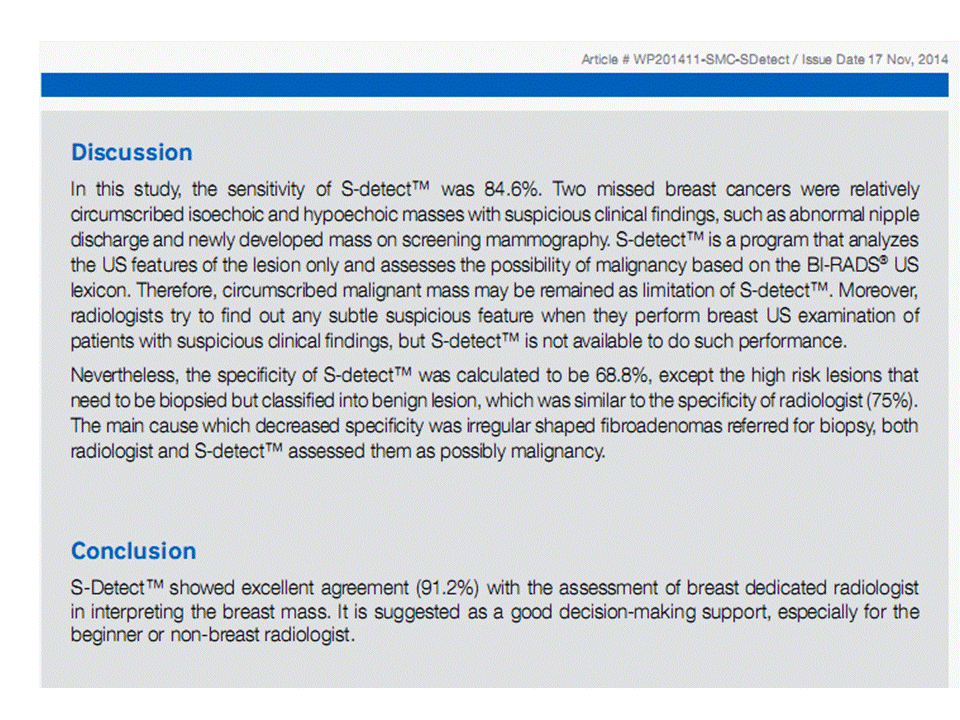
S-Detect In Breast Ultrasound on SAMSUNG RS80A
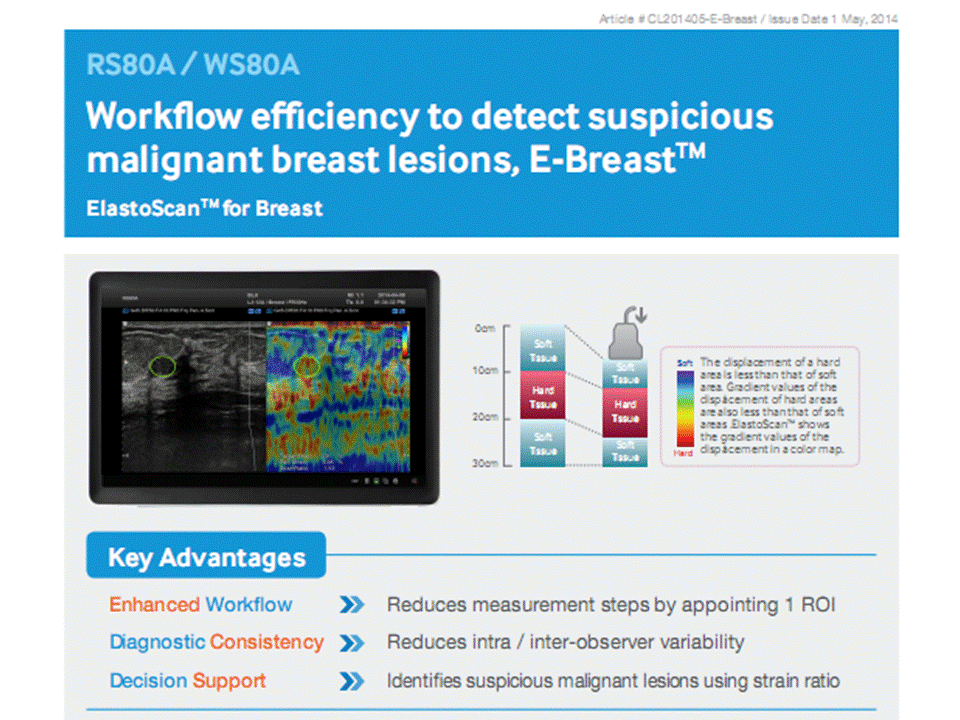
E-Breast™
A complementary diagnostic ultrasound technique for imaging elasticity, Elastography, noninvasively assesses the relative tissue stiffness of lesions compared to the stiffness of surrounding tissues to detect suspicious malignant lesions. Stiffer areas hardly deform than do their surroundings and provide dark contrast, whereas softer areas provide light contrast. This technique is normally used as an additional diagnostic tool to differentiate benign from malignant solid breast masses providing information on the mechanical properties, since malignant lesions are generally harder than benign lesions. Breast Elastography can substantially improve ultrasound capability in differentiating benign from malignant breast lesions with increased sensitivity and specifcity of breast ultrasound, thus reducing the number of biopsies. However, the limitation of the Elastography is the inter- /intra-observer variability and lack of standardized compression. To overcome these problems, Samsung Medison developed the semi-quantifcation ElastoScanTM technique, E-BreastTM(ElastoScanTM for Breast), using strain ratio which compares the strain of a region of interest and that of a reference region. E-BreastTM improves classifcation and characterization of benign and malignant breast masses.
Thứ Sáu, 17 tháng 4, 2015
Quantum Ultrasonics, Dr. Jason Birnholz
Practice of Ultrasound: Part 22 -- Quantum ultrasonics
By Dr. Jason Birnholz, AuntMinnie.com contributing writerApril 3, 2015
Fellow Ultrasounders,
I have never thought that ultrasound physics content for medical users has anything to do with either ultrasound or physics. As I see it, being rootless scientifically has limited the technical progress of our field, even while its clinical utilization and popularity have increased. It is as if we are all on the ultrasound supership on a medical ocean without a rudder.
Dr. Jason Birnholz.
Let's take an excursion to our parent realm, x-ray imaging. I hope many of you had a chance to visit the special exhibit at the last RSNA meeting, which celebrated the centennial of the organization. There were Crookes tubes, some of the first commercial radiography equipment, and lots of anecdotes by and about the field's pioneers.
There is mystery and magic in the scenery of an invisible beam that leaves a remnant of its silent passage through the body. The earliest users, like the earliest photographers, did not have much of a clue of what they were working with, obviously. They accomplished something magnificent, but real progress started when the physical foundations for x-ray work and the clinical goals of its users were integrated.
Photons
X-rays are streams of photons, sufficiently energetic that they can cause biologic harm. There were the sad lessons of early users with repeated exposures that taught us respect and operational restraint and also led to ways to intensify and channel those destructive effects as a surgical alternative or adjunct. Magic and mystery and danger: a captivating triad.
A photon is an energy packet. Visible light are streams of photons, and when you look up at a night sky, you have to be awed by the notion of these vanishingly tiny energy parcels, traversing interstellar and even intergalactic space, eternally, at a constant velocity.
At the end of the 19th century, Planck was working on a phenomenon called black-body radiation when he had an astounding insight: that energy is conveyed by individual packets. Extant data could all be modeled by each packet having a single, discrete energy. Considering each packet as a harmonic wave, he proposed that its energy was determined solely by its frequency and that each packet had just one discrete energy value. This was expressed by E = hν, where h is a constant and ν(Greek "nu") is frequency.
Planck's constant has a value of 6.62606957 × 10-34 m2 kg/s. Perhaps the most impressive aspect of Planck's concept was that in an intellectual world where everything mathematical was always on a continuous scale with an infinite number of gradations possible between any two numerical values, nobody ever thought in terms of discrete, fixed values for heat, light, or any form of energy. The former world was a place where everything was a little blurred at some level of magnification.
That is why his concept was so outside the box or beyond the silo (if the box metaphor seems clichéd). And if you wanted to test it experimentally, you would seem to need an impossible 34-place measurement precision. It's not a surprise that virtually all of the people who worried about such matters gave the notion a double thumbs down.
Around the same time, Einstein was working on a recently described phenomenon of generating an electric current by shining a light on a piece of metal. In one direction, you have a solar cell, and in the other, liquid crystal displays. Of course, no one could have known that then. However, his observations were definitely worth a Nobel Prize, because he found that generating current depended on the frequency (i.e., color) of light, not its intensity.
In the red-orange side of the spectrum, nothing happened, but a threshold was passed, and electrons were kicked out of their stable atomic locations at the higher frequency violet end of the visible light spectrum. This demonstrated the validity of the Planck supposition and jump-started the quantum era. Einstein also derived the Planck equation by an independent means. There was some later stuff about gravity and relativity too. He has always been my hero.
When you were thinking of light photons streaming across the galaxy, did you picture them as bullets? One of the problems of any technical field is that they borrow everyday words and then have to redefine them, and they always continue to suffer the weight of semantic overtones. Patients may complain of a medical vocabulary when it is not translated into common terms, but the words we use professionally convey a distinct meaning -- except when we want them to be ambiguous.
Early quantum physicists had a problem right at the start, because they could not resolve the issue of whether photons were waves or solid particles. For the most part, they were trying to explain experimental observations and resolve an irreconcilable linguistic difference at the same time. Compounding the problem rather than illuminating it were the immutable conservation laws: Energy is neither created nor destroyed; ditto for matter, charge, and momentum. (There is spin, too, but we're not going there.)
E=MC2, right? E is energy, M is mass, and C is the velocity of a photon in a vacuum, which is a constant. One way to think of a photon is that E/M is a constant and that what happens is a probabilistic, dynamic equilibrium shifting from mostly wave-like E to the mostly particulate M part that conveys momentum. When the photon at a high enough frequency encounters an electron, there will be an elastic collision. This is Compton scattering (1924), which is the atom-level interaction we use for x-ray imaging.
As particles, photons carry no charge. There is no antiphoton. As waves, photons with the same frequency can occupy the same space and time. Particles that have this property are referred to as "bosons." Photons consist of a stable pairing of a quark and antiquark; "waves" are something like a shimmering probabilistic field, instead of what we think of when we are watching the surface of an ocean.
A photon is the messenger of electromagnetism, one of the four basic forces that shape our universe. One of the ways of regarding photons is as an information tidbit. Seen this way, a photon coming within the field of an electron or proton conveys an instruction of what the larger object has to do. Keep this concept somewhere in the back of your mind for now.
6.0221413 × 1023
I assume you all recognize Avogadro's constant, which is the number of atoms in a mole of any substance. This was identified way back in 1811, a pretty humbling example of what simple observations and brain power can achieve. It's a mighty big number. One mole of water weighs 18.6 grams, a tad more than half an ounce. I remember hearing that there are more water molecules in a glass of water than there are glasses of water in all our oceans. Another example is that a mole stack of 1-inch donuts would extend from your morning coffee shop to a place about 1.6 million light years away, well beyond the Milky Way.
I'm mentioning this because we never deal with individual photons in our work or daily lives, but instead with mind-boggling numbers of them at any one time. A 100-watt bulb spouts out some 1020 photons every second. There are perhaps 1014 cells in the body, and each of those has scads of organelles, molecules, and atoms. It's easy to lose sight of the truly vast numbers of participants in an x-ray exposure, radionuclide scan, or one of our ultrasound imaging sessions.
Phonons
Like our x-ray-wielding cousins, we in ultrasound deal with photons too! E = hνapplies, as always. The energy packets that we use comprise the phonon part of the spectrum, and they have some special properties.
Photons of light, radio, and x-rays are identified as electromagnetic and are described as having out-of-phase harmonic electrical and magnetic oscillations. These all propagate through a vacuum at the speed of light, independent of frequency. Propagation velocity is less in solid media, proportional to its index of refraction: about two-thirds the speed of light in glass and about half C in diamond.
Light spread by a prism maps the energy level as frequency increases with each step of red, orange, yellow, green, blue, indigo, and violet (ROYGBIV). For oscillating waves, like all electromagnetic ones, one can characterize them on the basis of frequency, cycles per unit time, or wavelength, which is the length traversed by one cycle of a propagation wave in a medium. So f (instead of nu, to avoid confusion with v for velocity) = v/λ. Lambda is the symbol for wavelength, a value that is typically used for image-related work since you cannot resolve structures smaller than a wavelength. The wavelength for light is in the range of 5 × 10-7 m and for a 70-KeV x-ray photon, it is about 10-11 m; the size of a water molecule is 3 × 10-10 m.
Ultrasonic phonons are orders of magnitude less energetic than light and x-ray photons. They cannot propagate through a vacuum or gas. Atoms in a tight lattice of a crystal and molecules in a liquid are each vibrating in accord with their characteristic energy level. Phonons propagate as vibrational energy. There is a limiting frequency for vibration in solids that is about 1013 Hz, which is in the infrared domain and the point at which there is potential ionization in tissues, plainly not an issue for our weak but valiant lower frequency phonons.
Like their higher-energy cousins, phonons have an orthogonal, out-of-phase wave structure. Because they do not change the center of mass of oscillating atoms as they propagate, phonons do not have mass, are fully wave-like, and they are unaffected by gravity.
When a pure wave is dissipated, it is gone forever. Phonons can be created from more energetic photons after energy-depleting interactions. Under some conditions, phonons may cause inelastic diffraction of light photons, known as the Brillouin effect. There are some well-founded speculations that vibrational phonon interactions are an integral step in the energy transfer mechanism of photosynthesis.
Phonons are low-energy photons with a distinct identity, worthy of their own name. They can also be thought of as messengers of vibrational energy operating in a thermodynamic space rather than an electrodynamic domain, which includes chemical bonding for the molecules in the phonon landscape.
Who among us might not appreciate the cuteness or the grim determination of a single energy phonon gliding like heat through the molecular soup of some part of the body at just 0.00051% of the speed of an x-ray photon. It causes no damage. In its passage, it is jostled and bounced around over the mosh pit of a vast number of perpetually vibrating water molecules. Each water molecule has strong 104° oxygen hydrogen bonds within itself and two hydrogen bonds to adjacent water molecules. Two of the bonds are short and two are long.
The phonon contributes to this bond-length dance and is reinforced by it. At some point it smacks up against a wall bigger than its wavelength and is sent off on another rave along a new trajectory. Substitute triple-stranded superhelices of collagen for the generic "wall" and you have the essence of what information is conveyed to us by our dogged traveler.
The next step
Ultrasound has always struggled academically and intellectually, because we have collectively not understood that our foundations have a basic commonality with the older and more familiar, higher energy, photon-based forms of body imaging. This has a lot to do with status of the method, when it is selected for use, and our pride in using it.
We urge our patients to become better informed and interact with their care providers, including those times when an imaging study is on the diagnostic menu. The global, medical ultrasound community has not been as diligent in educating itself about the intricacies of what we do. Can we continue to rely on stolid-state physics?
I used to ask audiences about where ultrasound comes from, expecting sonar as the common answer. The answer I would have liked to have heard, even once, was the physical exam technique of percussion. As you know, this was used initially on wine vats and then on chests. Rapping briskly with a finger and either feeling the vibrations or listening for the sound is no different from smashing a quartz crystal underwater and listening or otherwise sensing acoustic reverberations from an iceberg or submarine. We do things a lot better now than when I made my own first ultrasound images in 1968, but we pretty much all do it the same way now that we did then.
In the real world, we deal with aggregated beams of gazillions of phonons traversing a medium that is far from ideal. Put another way, lack of coherence of the acoustic signals for interrogating tissues makes for a whole lot of noise in the images we have to work with. Think about this and do a search for the term "SASER." That is an example of how integrating our phononic foundations will shape our future. Phonons are ultralovely heirs of their magical, mysterious, and dangerous relatives whose potential is yet to have been exploited fully.
Dr. Jason Birnholz was one of the few advanced academic fellows of the James Picker Foundation, and he has been a professor of radiology and obstetrics. He is a fellow of the American College of Radiology and the Royal College of Radiology, and he was an associate fellow of the American College of Obstetricians and Gynecologists.
The comments and observations expressed herein do not necessarily reflect the opinions of AuntMinnie.com.
Related Reading
Copyright © 2015 AuntMinnie.com
Last Updated er 4/2/2015 9:16:29 PM
Forum Comments
Thứ Bảy, 11 tháng 4, 2015
Đăng ký:
Bài đăng
(
Atom
)